Association Between Uric Acid Levels and Stenosis Severity in Patients With and Without Renal Insufficiency
Keywords:
Hyperuricemia, Coronary artery disease, renal insufficiency, acute coronary syndrome,, angiographyAbstract
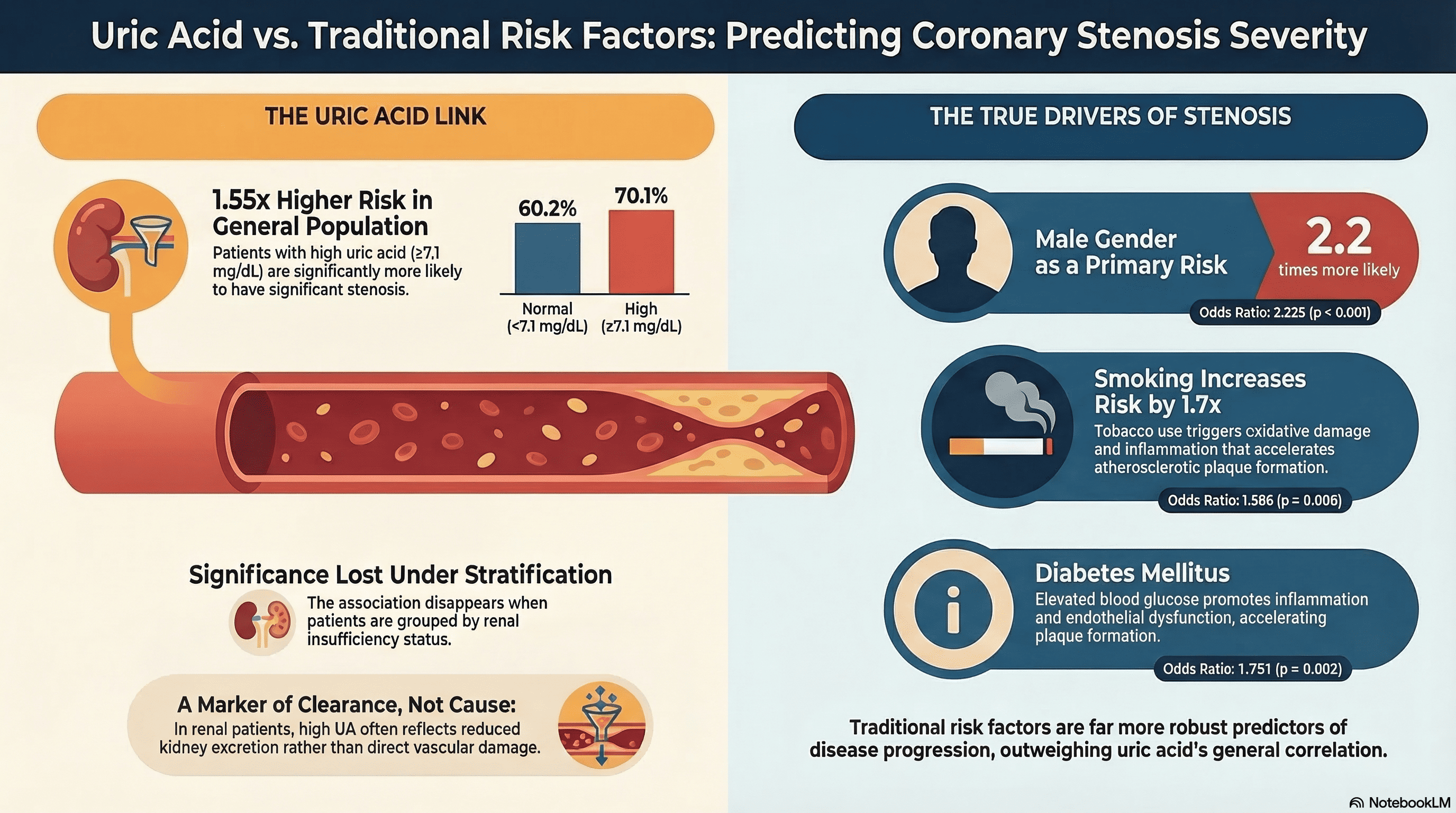
Hyperuricemia is associated with an increased risk of atherosclerosis and coronary stenosis, particularly in the presence of renal insufficiency. However, the independent relationship between serum uric acid levels and the severity of coronary stenosis, when stratified by renal function, remains poorly understood. This study aimed to evaluate the association between serum uric acid concentrations and the extent of coronary stenosis in patients with and without renal insufficiency. A cross-sectional study was conducted on 853 patients diagnosed with acute coronary syndrome (ACS) who underwent coronary angiography. Elevated uric acid was defined as ≥ 7.1 mg/dL, while renal insufficiency was defined as an estimated glomerular filtration rate (eGFR) < 60 mL/min/1.73 m². The associations between variables were analyzed using Chi-square tests and logistic regression models. The 853 patients, 386 (45.3%) presented with renal insufficiency. In the overall cohort, elevated uric acid levels were significantly associated with coronary stenosis of 50% or greater (p = 0.005). However, upon subgroup analysis, this association lost statistical significance in both the renal insufficiency (p = 0.319) and non-renal insufficiency (p = 0.154) groups. Conversely, traditional cardiovascular risk factors—specifically advanced age (p < 0.001), male sex (p < 0.001), and smoking history (p = 0.008)—remained significantly associated with coronary stenosis across both subgroups. While elevated serum uric acid levels correlate with coronary stenosis in the general ACS population, this relationship does not remain independently significant when patients are stratified by renal function. Traditional risk factors, such as age, sex, and smoking, serve as more robust predictors for the progression of coronary stenosis.
Downloads
References
Badan Penelitian dan Pengembangan Kesehatan. RISKESDAS. Jakarta; 2018.
Neumann F-J, Sousa-Uva M, Ahlsson A, et al. 2018 ESC/EACTS Guidelines On Myocardial Revascularization. European Heart Journal. 2019;40(2):87–165.
Kuwabara M, Kuwabara R, Hisatome I, et al. “Metabolically Healthy” Obesity And Hyperuricemia Increase Risk For Hypertension And Diabetes: 5‐year Japanese Cohort Study. Obesity. 2017;25(11):1997–2008.
Muiesan ML, Agabiti-Rosei C, Paini A, Salvetti M. Uric Acid and Cardiovascular Disease: An Update. Eur Cardiol. 2016 Aug;11(1):54-59. doi: 10.15420/ecr.2016:4:2. PMID: 30310447; PMCID: PMC6159425.
Lee, T.H.; Chen, J.-J.; Wu, C.-Y.; Yang, C.-W.; Yang, H.-Y. Hyperuricemia and Progression of Chronic Kidney Disease: A Review from Physiology and Pathogenesis to the Role of Urate-Lowering Therapy. Diagnostics 2021, 11, 1674. https://doi.org/10.3390/diagnostics11091674
Vargas-Santos AB, and Neogi T. Management Of Gout And Hyperuricemia In CKD. American Journal of Kidney Diseases. 2017;70(3):422–39.
Yang B, Ma K, Xiang R, et al. Uric Acid And Evaluate The Coronary Vascular Stenosis Gensini Score Correlation Research And In Gender Differences. BMC Cardiovascular Disorders. 2023;23(1).
Caliceti C, Calabria D, Roda A, and Cicero A. Fructose Intake, Serum Uric Acid, And Cardiometabolic Disorders: A Critical Review. Nutrients. 2017;9(4):395.
Yamagishi S, Ishibashi Y, Ojima A, Sugiura T, and Matsui T. Linagliptin, A Xanthine-Based Dipeptidyl Peptidase-4 Inhibitor, Decreases Serum Uric Acid Levels In Type 2 Diabetic Patients Partly By Suppressing Xanthine Oxidase Activity. International Journal of Cardiology. 2014;176(2):550–2.
Burnstock G. Purinergic Signalling And Endothelium. Current Vascular Pharmacology. 2016;14(2):130–45.
Zalawadiya SK, Veeranna V, Mallikethi-Reddy S, et al. Uric Acid And Cardiovascular Disease Risk Reclassification: Findings From NHANES III. European Journal of Preventive Cardiology. 2015;22(4):513–8.
White J, Sofat R, Hemani G, et al. Plasma Urate Concentration And Risk Of Coronary Heart Disease: A Mendelian Randomisation Analysis. The Lancet Diabetes & Endocrinology. 2016;4(4):327–36.
Maloberti A, Bossi I, Tassistro E, et al. Uric Acid In Chronic Coronary Syndromes: Relationship With Coronary Artery Disease Severity And Left Ventricular Diastolic Parameter. Nutrition, metabolism, and cardiovascular diseases : NMCD. 2021;31(5):1501–8.
Kleber ME, Delgado G, Grammer TB, et al. Uric Acid And Cardiovascular Events. Journal of the American Society of Nephrology. 2015;26(11):2831–8.
Filipa Alexandre A, Stoelzel M, Kiran A, Garcia-Hernandez A, Morga A, and Kalra PA. Clinical Factors For Predicting Cardiovascular Risk, Need For renal Replacement Therapy, And Mortality In Patients With Non–Dialysis-Dependent Stage 3–5 Chronic Kidney Disease From The Salford Kidney Study. Journal of Nephrology. 2023;36(6):1639–49.
Lee, T.H.; Chen, J.-J.; Wu, C.-Y.; Yang, C.-W.; Yang, H.-Y. Hyperuricemia and Progression of Chronic Kidney Disease: A Review from Physiology and Pathogenesis to the Role of Urate-Lowering Therapy. Diagnostics 2021, 11, 1674. https://doi.org/10.3390/diagnostics11091674.
Culleton BF, Larson MG, Kannel WB, Levy D. Serum uric acid and risk for cardiovascular disease and death: The Framingham Heart Study. Ann Intern Med. 1999;131(1):7-13. doi: 10.7326/0003-4819-131-1-199907060-00003.
Cubrilo M, Banovic M, Matkovic M, et al. Incidence And Prognostic Significance Of Silent Coronary Disease In Asymptomatic Patients With Severe Aortic Stenosis. Medicina. 2024;60(9):1503.
Xiang D, Liu Y, Zhou S, Zhou E, and Wang Y. Protective Effects Of Estrogen On Cardiovascular Disease Mediated By Oxidative Stress. Oxidative Medicine and Cellular Longevity. 2021;2021(1).
Gallucci G, Tartarone A, Lerose R, Lalinga AV, and Capobianco AM. Cardiovascular Risk Of Smoking And Benefits Of Smoking Cessation. Journal of Thoracic Disease. 2020;12(7):3866–76.
Steven S, Frenis K, Oelze M, et al. Vascular Inflammation And Oxidative Stress: Major Triggers For Cardiovascular Disease. Oxidative Medicine and Cellular Longevity. 2019;2019:1–26.
Fresán U, Guevara M, Trobajo-Sanmartín C, Burgui C, Ezpeleta C, and Castilla J. Hypertension And Related Comorbidities As Potential Risk Factors For COVID-19 Hospitalization And Severity: A Prospective Population-Based Cohort Study. Journal of Clinical Medicine. 2021;10(6):1194.
Saeed D, Reza T, Shahzad MW, et al. Navigating The Crossroads: Understanding The Link Between Chronic Kidney Disease And Cardiovascular Health. Cureus. 2023;
Published
How to Cite
Issue
Section
Copyright (c) 2026 M Saugi Abduh , Muh Adytia Prasada, Ahmad Umar Alfaruq, Dimas Irfan Nabih

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.




















