Correlation Between Hydration Status and Renal Ultrasonographic Parameters: A Cross-Sectional Study
Keywords:
Renal Ultrasonography, Parenchymal Echogenicity, Hydration Status Assessment, Perceived Urine-Richness Index (PURI)Abstract
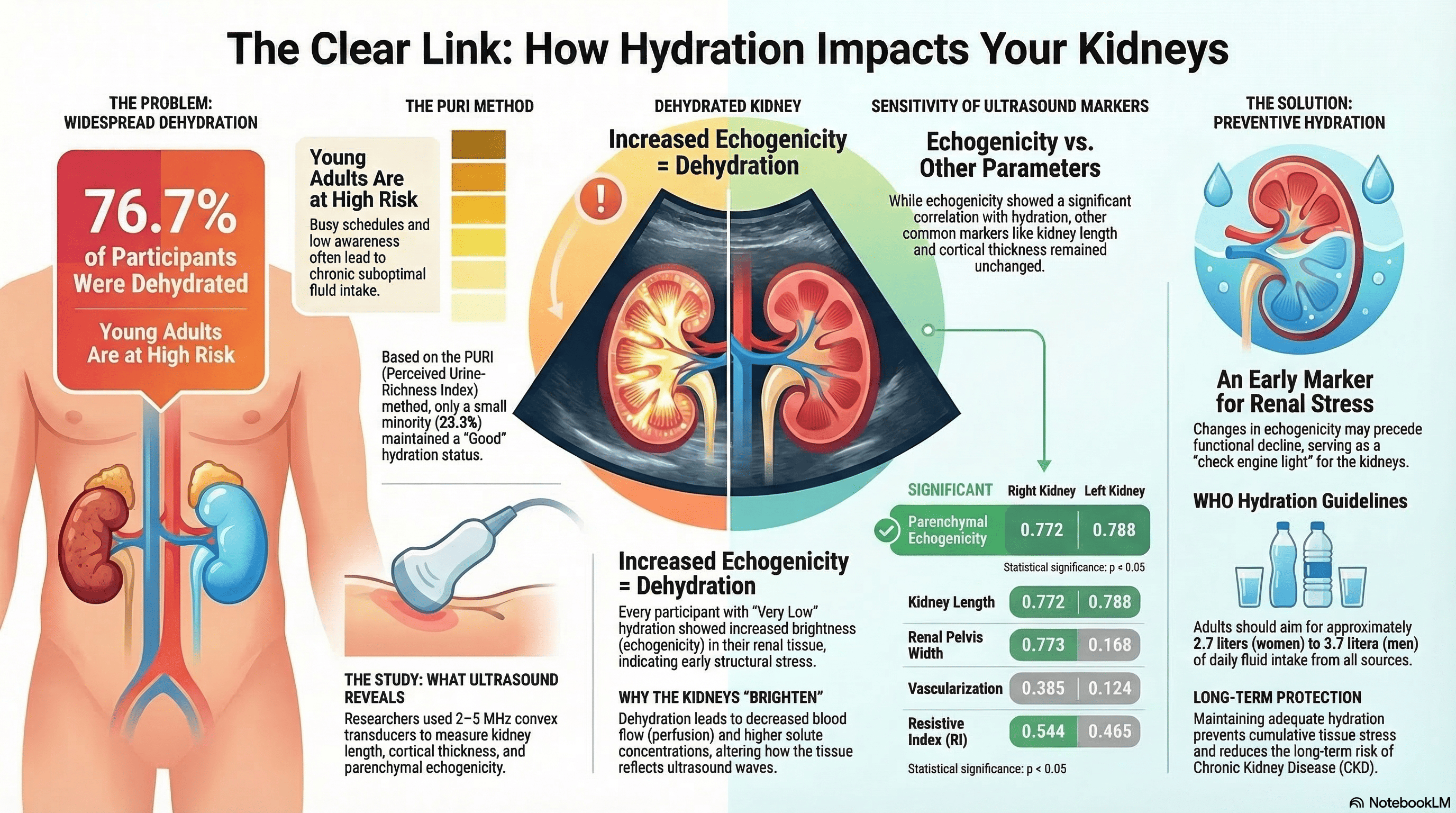
The kidneys play a critical role in maintaining fluid homeostasis, and suboptimal hydration may lead to morphological alterations detectable via imaging. This study aimed to analyze the correlation between hydration status and various renal ultrasonographic parameters. An observational, cross-sectional study was conducted with 30 healthy radiology students selected through purposive sampling. Hydration status was evaluated using the Perceived Urine-Richness Index (PURI) based on morning urine color. Renal ultrasound examinations were performed to assess kidney size, parenchymal echogenicity, corticomedullary differentiation, and resistive index. Data were statistically analyzed using the Chi-Square test with a significance threshold of p<0.05. The assessment revealed that 76.7% of participants had low to very low hydration levels. Statistical analysis demonstrated that parenchymal echogenicity was the only parameter significantly correlated with hydration status (p=0.001 for the right kidney; p=0.004 for the left kidney). Other ultrasonographic markers, including kidney length, cortical thickness, and resistive index (RI), showed no significant association with hydration levels. Hydration status is significantly associated with changes in renal parenchymal echogenicity, identifying it as a sensitive, non-invasive marker for early renal stress and subclinical morphological changes. These findings underscore the necessity of maintaining adequate fluid intake to preserve renal structural integrity as visualized through ultrasonography.
Downloads
References
Dalal R, Bruss ZS, Sehdev JS. Physiology, Renal Blood Flow and Filtration. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 [cited 2026 Mar 16]. Available from: http://www.ncbi.nlm.nih.gov/books/NBK482248/ PubMed PMID: 29489242.
Seal AD, Suh HG, Jansen LT, Summers LDG, Kavouras SA. Hydration and Health. Analysis in Nutrition Research: Principles of Statistical Methodology and Interpretation of the Results. Elsevier Inc.; 2019. 299–319 p. doi:10.1016/B978-0-12-814556-2.00011-7
Imenez Silva PH, Mohebbi N. Kidney metabolism and acid–base control: back to the basics. Pflugers Archiv European Journal of Physiology. 2022;474(8):919–34. doi:10.1007/s00424-022-02696-6 PubMed PMID: 35513635.
Mrs. Shrutika D. Adkine ST, AP. Kidney And Dialysis With Its Complications And Management. Journal of Pharmaceutical Negative Results. 2022;13(8):178–84. doi:10.47750/pnr.2022.13.S08.27
Myram S. Development of a biomimetic multitube system for the study of ADPKD To cite this version : HAL Id : tel-04643279 Sorbonne Université pour l ’ étude de l ’ ADPKD. 2024.
Ummah MS. Anatomi, Fisiologi dan Histologi Ginjal. Sustainability (Switzerland). 2019;11(1):1–14. PubMed PMID: 25246403.
Rahmayati E, Sari G, Heru Apriantoro N, Dimas Prayogi U, Irwan D, Restiyanti Y, et al. Gambaran Morfologi Usg Ginjal Dengan Kreatinin Tinggi Pada Kasus Gagal Ginjal Kronik. Kocenin Serial Konferensi. 2021;1(1):1–7.
Gao J., Thai, A., Lee, J., & Fowlkes JB. Ultrasound Shear Wave Elastograhy and Doppler Sonography to Assess the Effect of Hydration on Human Kidnes: a Preliminary Observation. 2020.
Bartram J, William. Domestic Water Quantity , Service Level and Health, second edition. World Health Organization. 2020. 76 p.
Alam S, Majid NI. Nutritional Status, Physical Activity, and Fluid Intake with Dehydration Status of Farmers in Jeneponto Regency. Al GIZZAI: Public Health Nutrition Journal. 2023;III(1):43–51. doi:10.24252/algizzai.v3i1.35768
Garrett DC, Rae N, Fletcher JR, Zarnke S, Thorson S, Hogan DB, et al. Engineering Approaches to Assessing Hydration Status. IEEE Reviews in Biomedical Engineering. 2018;11(c):233–48. doi:10.1109/RBME.2017.2776041 PubMed PMID: 29990109.
Reber E, Gomes F, Dähn IA, Vasiloglou MF, Stanga Z. Management of dehydration in patients suffering swallowing difficulties. Journal of Clinical Medicine. 2019;8(11). doi:10.3390/jcm8111923
Karakosta P. Comparative analysis between rapid evaluation algorithm and finite differences approximations solution for the Pennes Bioheat Equation Supervised by Professor Theodoros Samaras. 2020.
Roumelioti ME, Glew RH, Khitan ZJ, Rondon-Berrios H, Argyropoulos CP, Malhotra D, et al. Fluid balance concepts in medicine: Principles and practice. World Journal of Nephrology. 2018;7(1):1–28. doi:10.5527/wjn.v7.i1.1
Yang X, Wu H, Li H. Dehydration-associated chronic kidney disease: A novel case of kidney failure in China. BMC Nephrology. 2020;21(1):1–5. doi:10.1186/s12882-020-01804-x PubMed PMID: 32366263.
Nurmurzaev Z.N., Suvonov Z.K. KIKh. Ultrasound of the Abdominal Cavity. 2023;6.
Miesner M. Abdominal Ultrasound. Veterinary Techniques in Llamas and Alpacas, Second Edition. 2023. 152–156 p. doi:10.1002/9781119860792.ch37
Herawati E, Wijayanti ET. Uji PURI Sebagai Gambaran Status Hidrasi Jangka Pendek Selama Jam Kuliah Pada Mahasiswa. Biofaal Journal. 2023;4(2):090–9. doi:10.30598/biofaal.v4i2pp090-099
Dewi Aryanti, Triguna Y. Status Hidrasi pada Mahasiswa dan Pekerja: Studi Komparasi. Media Informasi. 2024;20(1):9–15. doi:10.37160/mijournal.v20i1.442
O’Boyle MK. Color Atlas of Ultrasound Anatomy. American Journal of Roentgenology. 2005. 1371–1371 p. doi:10.2214/ajr.184.4.01841371
Diwakar RK. Basics of Abdominal, Gynaecological, Obstetrics and Small Parts Ultrasound. Basics of Abdominal, Gynaecological, Obstetrics and Small Parts Ultrasound. 2018. doi:10.1007/978-981-10-4873-9
Chapman, C.L., Holt, S.M., & O’Connell CT. Acute kidney injury biomarkers and hydration assessments following prolonged mild hypohydration in healthy young adults. American Journal of Physiology-Renal Physiology. 2023.
Radic, J., Kolak, E, Vuckovic, M, Gelemanovic, A., & Dogas H. Assessment of hydration, nutritional status and arterial stiffness in hyertensive chronic kidney disease patients. Nutrients, 15(9), 2045. 2023.
Qian G, Liu C, Guo J, Dong W, Wang J, Chen Y. Prevention of contrast‐induced nephropathy by adequate hydration combined with isosorbide dinitrate for patients with renal insufficiency and congestive heart failure. Clin Cardiol. 2019 Jan 7;42(1):21–5. doi:10.1002/clc.23023 PubMed PMID: 30054906; PubMed Central PMCID: PMC6436482.
Dakio F, Idris N, Muis M, Alfian A, Kasim H, Murtala B. the Correlation Between the Size of Cortex Thickness and the Resistive Index of Kidney Based on Ultrasonography Examination in Hydronephrosis Patients. A Scientific Journal. 2019;12(2):183–93. doi:10.20884/1.mandala.
Published
How to Cite
Issue
Section
Copyright (c) 2026 Wahyu Hidayat, Nurbaiti Nurbaiti, Sriyatun Sriyatun, Puji Supriyono, Minda Fitrah Riwanda, Puspa Pamella Suci

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.




















